Headlines
- Gentle Daily Ear Care with Medicare Ear Spray
- Breathe Easy with Medicare Nasal Spray
- Fleming Medical Renews Support for Irish Heart Foundation’s “Before Damage is Done” Campaign with over €25K Donation
- First Response for Minor Burns: Why MD508 Medicare Burn Spray Belongs in Every Medicine Cabinet
- Step Smart: Introducing the New Medicare® Footcare Range
Watch the Recording: Asthma & Allergy Webinar with Dr Dorothy Ryan, Respiratory Consultant
21 June 2021

Following the success of the Wound Care webinar in March, Fleming Medical also presented an Asthma and Allergy Awareness webinar on the 25th of May. Watch the recording here.
They were joined on the webinar by Dr. Dorothy Ryan from Beaumont Hospital, who is an expert in respiratory conditions with a specialty interest in airways diseases - severe asthma and bronchiectasis.
Her presentation took a case-based approach to highlight the challenges in diagnosing and managing uncontrolled and severe asthma, with particular emphasis on the use of exhaled nitric oxide (FeNO) in guiding use of inhaled corticosteroids in asthma.
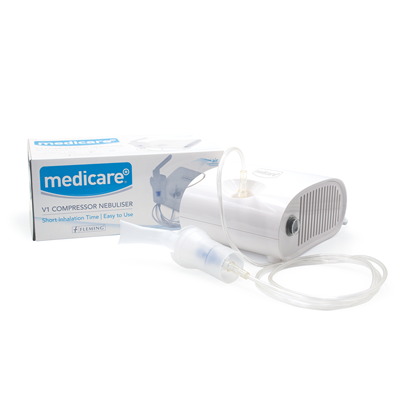
James Reihill, Clinical Training Specialist at Fleming Medical, who also hosted the training explored some of the devices related to asthma like spirometers and nebulisers as well as how to manage allergies at home.
If you would like to watch the recording, click below:
Watch Now
Here are some valuable insights that arose from the webinar with Dr Ryan:
Asthma Triggers & Inducers
Asthma is characterised by variable airflow obstruction and to diagnose this, you would need to use spirometry or a peak flow diary that patients complete.The difference between triggers and inducers is that triggers worsen symptoms and inducers cause acute exacerbation (asthma attacks).
Triggers are mostly inhaled and won’t cause an acute exacerbation of asthma but can worsen symptoms.
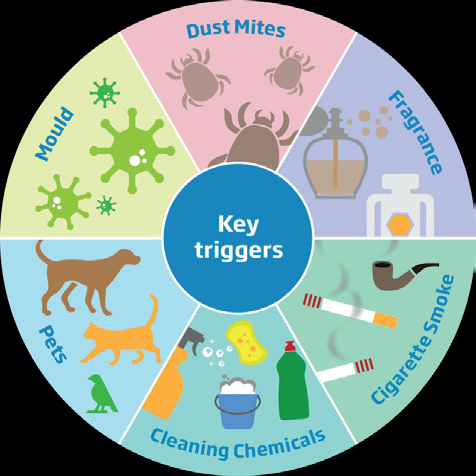
Each person has their own inducers and triggers specific to them, but viral respiratory infections are a massive problem for asthma sufferers. Dr Ryan explained how the recent pandemic has impacted respiratory infections:
“At Beaumont Hospital, we have seen a 40% reduction in asthma admissions to the hospital throughout the pandemic and that is hugely because patients are keeping their distance, wearing their masks, using their alcohol hand gel. All the common viral inducers of asthma exacerbations have gone away during that time. We had very little flu and it is a nice learning point for patients going forward”.
Atopy & Asthma
Atopy is the tendency for a person to develop antibodies to specific Immunoglobulin Es (IgE). Atopy is very prevalent, 1 in 3 of the population have it, 1 in 6 people will have symptoms such as hay fever.Dr Ryan explored atopic asthma which is the type of asthma that is triggered by allergens such as pollen, house dust mites, pet dander, etc. 1 in 12 of the population will have atopic asthma.
Allergen groups:
- Pollen
- Fungal Spores, such as Aspergillus
- Animal dander
- House dust mite/insects (HDM)

House Dust Mites & Asthma
Asthma patients are often unaware that they are dust mite sensitive, the reason for this is that there isn’t a huge amount of them in the air. They are embedded into soft furnishings and classically thrive in mattresses and pillow and duvet covers. People are not aware of the effects of house dust mites as it occurs mostly when you sleep, and you are chronically exposed to it so you don’t have severe acute symptoms. Even vigorous cleaning can bring house dust mites into the air so asthmatics should not clean, soft furnishings themselves as it can further trigger them.
Regular vacuuming is recommended for rooms with carpets in them as house dust mites can go from the floor to the bed. Ensure that your vacuum has a HEPA filter. If you have carpets, steam cleaning is another way you can combat house dust mites.
Pet Dander & Asthma
60% of asthma patients are pet allergic with 33% of sensitised patients living with a pet. It is advised that asthma sufferers do not own pets, however, if a person develops asthma and already has a pet, regular cleaning and vacuuming must occur. Again, this cannot be carried out by the person who has asthma. Keep pets out of the main living area and bedroom and ensure you have a HEPA-filter air cleaners in these areas. Wash the pet as often as possible to help with shedding.
Asthma & Genetics
Not everybody is susceptible to inhaled allergens. Asthma is a very genetically dominant condition.A person may develop asthma if they are a genetically predisposed individual who then gets exposed to an allergen early or late in life. The person is more likely to develop asthma due to ongoing chronic exposure to the allergen.
Studies have been carried out where they have shown the level of house dust mite in a household, and they have found that the risk of house dust mite-sensitised children having asthma doubled for every doubling of house dust mite in their environment.
Questions & Answers
Participants in the webinar were invited to ask questions. We have compiled some of the questions below:How would asthmatics avoid the increasing pollen count in the summer months? Are antihistamines enough?
This is a huge challenge with a majority of allergens, they are not avoidable. Patients can try to control House Dust Mite but ultimately you cannot eradicate it or avoid it completely. It is very difficult to place ourselves in a bubble during spring, summer and autumn. What’s interesting with social distancing and wearing masks that is has helped asthmatics but it not socially acceptable after the pandemic is over. In terms of avoiding pollen, try to get an antihistamine prescribed ahead of the season that they are particularly allergic to. I would often recommend starting a month ahead and take regularly throughout the season which is a trigger for patients. That can offset some of the symptoms. Make sure you don’t cut the grass or do gardening if you can.
Is it possible that strong smells affect asthma?
Inhaled irritants can affect some asthmatics, not so much strong smells from food. When we are talking about inhaled irritants, we mean predominantly sprays, perfumes, cleaning agents, chemicals that have molecules of a certain size that you breathe in. Spicy foods can trigger coughs. Where strong smells are impactful are in asthmatics who have vocal cord disfunction. That is a separate diagnosis which is mostly found in young females with asthma.
What should you do when someone has an asthma attack?
Acute asthma attacks are quite frightening. The best thing to do is to try to get that person to a hospital as quickly as possible. Make sure they get as much of the blue inhaler into them as possible. Ideally, if you have a spacer device, it is the best way for them to get it down into their lungs because technique with meter dose inhalers is tricky, if they are struggling to breathe it is even worse again.
I have heard that mild asthma may improve over the years, is this true?
What we see mostly is if people have childhood asthma, they can grow out of it. If asthma occurs as an adult or if childhood asthma comes back, that tends to stay. Over a quarter of asthma is in patients over 25 years old from people who have had no history of childhood asthma. As an adult, it will more than likely stay but it can still be mild, and they may not need treatment at that stage.

 Fleming Medical UK
Fleming Medical UK